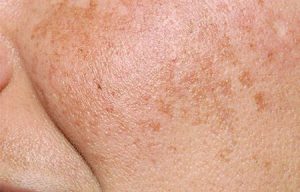
The Causes and Treatment of Adult Acne

The Causes and Treatment
of Adult Acne
written by Dermatologist, Dr Kesiree Naidoo

- The Causes and Treatment
- of Adult Acne
- What causes adult acne?
- Are there any tests needed to diagnose adult acne?
- How is acne treated?
- Topical Acne Treatments
- Retinoids
- Topical antibiotics
- Benzoyl peroxide
- Azelaic acid
- Topical combination treatments
- Systemic treatments
- Antibiotics
- Hormones
- When would I choose to prescribe a hormonal treatment?
- Cyproterone acetate
- Spironolactone
- Isotretinoin
- Cosmeceutical skincare
- Procedures
- Chemical peels
- Photodynamic therapy (PDT)
- Dermal needling
Adult acne also known as late onset or post adolescent acne has been the anguished subject of many dermatology room consults worldwide. Its diagnosis is almost always followed by questions like ‘Why do I still have acne now? ‘or ‘Aren’t I too old to get Acne’ or sometimes statements like ‘I’ve never had acne before’ or ‘I’ve always had a perfect skin till now’.
Sadly, adult acne is a continuous challenge, especially as it is difficult to treat with an often prolonged and recurrent course. It has become increasingly more common in recent years for leading dermatologists to question whether there are different factors playing a role as opposed to those causing adolescent acne.
Adult acne is defined as acne that affects men and women over the age of 25. It is by far more common in women than men. Adult acne may persist continuously from adolescence, recur after age 25 or in fact occur for the first time after the age of 25 years old. So, to answer those questions ‘Yes, you can still have acne beyond adolescence’ and ‘yes it can be for the first time’. Most cases of adult acne persist from adolescence and only around 20 % occurs for the first time after the age of 25. Hence the term adult acne seems more appropriate than late onset acne.
Traditionally it is believed that the main factors causing adult acne are genetic and hormonal, with predominant involvement of the lower third of the face. Flare-ups are typically premenstrual supporting the role of hormones. Most patients complain of deep seated and painful nodules with very few comedones (blackheads and whiteheads). The acne nodules are usually sparse, but can lead to significant scarring.
There are now considered to be 2 predominant forms of adult acne, inflammatory and retentional:
Inflammatory acne is the most common type accounting for 50-60% of cases. The skin is not always oily, and in fact may be normal to dry making it sensitive to topical treatments generally prescribed in adolescent acne. The acne spots can be on multiple areas and not just the lower third of the face.
Retentional acne is the other predominant subtype and is characterised by increased sebum or oily skin and multiple comedones (blackheads and whiteheads).
What causes adult acne?
The fundamental factors causing acne whether adolescent or adult are:
- Genetic predisposition. As many as 40% of acne sufferers have a family history of acne. This may be related to the size, number and activity of sebaceous glands which are genetically determined.
- Increased androgenic hormone (testosterone, dehydroepiandrosterone sulphate and dihydrotestosterone) stimulation of the sebaceous glands leading to an oily skin. The levels of the androgen need not be higher than normal. It is the sebaceous glands that are more responsive to normal levels of circulating androgens. Oestrogen inhibits the secretion of androgenic hormones and inhibits sebaceous gland activity. An age related decline in oestrogen tips the balance towards androgenic stimulation.
- Excessive sebum production by sebaceous glands. While this is largely driven by androgenic hormones, there are other factors that also stimulate the sebaceous glands.
- Abnormal follicular keratinisation leading to blocked pilosebaceous unit (hair follicle unit) and the formation of a comedones. The skin cells in the hair follicle do not shed easily. They accumulate and together with the increased sebum from the sebaceous glands block the opening of the follicle. This in turn contributes to the inflammatory response.
- Propionibacterium acnes or cutibacterium acnes which live normally in the sebaceous glands proliferate with increased sebum production worsening the inflammatory response and acne
- an inflammatory response primarily to Propionibacterium or cutibacterium acnes which release enzymes that trigger the inflammatory cascade. These cause papules and pustules in acne that we commonly refer to as ‘pimples’.
There are however other factors or triggers that may be more significant in causing adult acne and these need to be further evaluated:
Ultraviolet light exposure- excessive sun exposure causes thickening of the stratum corneum and accumulation of dead surface skin cells. There is stimulation of the sebaceous glands producing more sebum. Both these processes lead to comedones and acne
Stress- a stressful lifestyle with poor sleep patterns can cause acne by its effects on the pituitary adrenal axis and resultant release of corticotrophin releasing hormone, neuropeptides and proinflammatory cytokines which stimulate the sebaceous glands and worsen the inflammatory response.
Obesity and insulin resistance is associated with hormonal imbalance and acne.
Endocrine disorders – There are numerous endocrine diseases that cause acne by increasing the activity of androgens, stimulating the sebaceous glands or inducing abnormal keratinization. The most common cause is polycystic ovarian syndrome aka PCOS. Other conditions include congenital adrenal hyperplasia, hypothyroidism, Cushings syndrome and various other adrenal and ovarian tumours. Acne also occurs in menopause due to the decline in oestrogen and resultant increasing effects of male hormones.
Smoking – causes acne by stimulating the sebaceous glands and inducing abnormal keratinization. The acne associated with smoking is typically a non-inflammatory, comedomal acne. There are mainly blackheads and whiteheads without significant papules and pustules.
Diet -does diet worsen acne? There is not much scientific evidence, but studies have shown that high glycaemic index foods increase insulin and insulin like growth factor 1(IGF1) which stimulate the production of androgens and sebum.
In addition, diets rich in dairy products and muscle building supplements with whey protein have also been found to worsen acne. Anabolic steroids used by weight lifters and body builders can cause a severe scarring acne affecting the face and body.
Damage to the skin barrier – Over washing of the skin leading to a damaged epidermal skin barrier which in turn causes water loss through the skin and worsens the inflammatory cascade.
Greasy cosmetics – Occlusive makeup, Vaseline and other thick greasy creams block the follicles and cause acne in those that are susceptible. This problem is sometimes seen in actors and models or those requiring heavy make up as part of their job. Hair products that spreads onto the hairline can cause acne in the affected areas.
Medication- Some drugs can cause acne as a side effect. Examples of these drugs are progesterone only contraception (includes commonly used injectable contraception) benzodiazepines, mood stabilisers like lithium and blood pressure medication like ramipril. There is also some speculation as to whether hormone releasing intrauterine contraceptive devices and contraceptive implants possibly trigger acne in some women who are predisposed. Anabolic steroids used by weight lifters and body builders can cause a severe scarring acne affecting the face and body.
Are there any tests needed to diagnose adult acne?
Acne is a clinical diagnosis and lab tests are not needed to make the diagnosis. Even though androgenic (male) hormones are one of the main pathogenetic factors causing acne there is usually no increase in hormone levels. It is rather the balance between androgenic hormones and oestrogen that causes acne.
Investigations may be required if endocrine disorders associated with acne are suspected, though these conditions will usually have other signs and symptoms to warrant further investigation.
Polycystic ovarian syndrome (PCOS) commonly presents with acne as well as other signs of hyperandrogenism (increased male hormones). It is the most commonly suspected cause of adult female acne. PCOS will need laboratory investigations and abdominal imaging and a visit to the gynaecologist or endocrinologist.
How is acne treated?
This is the most difficult part.
Adult acne is challenging as it typically responds to treatment, but frequently recurs once treatment is stopped. Acne is also of varying severity and is sometimes not even present at the time of the dermatology consult. This is frustrating for both the patient and the dermatologist. Prolonged courses of treatment are often needed as well as rotating different treatment options, and off course maintenance treatment is essential, which often involves a good skincare regimen. We also have to take into account the possibility of pregnancy and breastfeeding which decreases treatment options. Adult patients tend to have a drier skin compared to adolescents which does not always tolerate topical prescription acne medication. There is really no one size fits all approach and each person needs to be evaluated individually and treated accordingly.
I am often asked for ‘the best treatment ‘or the ‘strongest treatment’. Patients are sometimes under the impression that it is possible to ‘treat acne and get it right the first time’. Sadly, the truth is there is no quick fix for adult acne. If there were.
- You would probably know about it
- Doctors would give it to you and there would not be more than that 1 treatment option
- You would not see so many people walking around with adult acne
Treatment options can be broadly divided into topical, systemic treatments, skincare and procedures.
Topical Acne Treatments
Topical treatments are best suited to mild to moderate acne and sporadic lesions. In this case they can be used as a spot treatment as needed. Topical treatments are also an important part of maintenance treatment.
Retinoids
Retinoids used for topical treatment include 0.1% adapalene gel( Differin, Dapta), and tretinoin( Retin -A, Ilotycin -A,Retacnyl) 0.05% cream and 0.025% gel.
These treatments are also fundamental to adolescent acne. Gradual introduction is recommended. Interestingly retinoids are also anti-ageing and prevent skin cancer. As mentioned, these topical treatments cause dryness and irritation of the skin in the first few weeks of use. They also cause photosensitivity. They must be used with a good moisturiser for skin hydration and comfort and with sunscreen over moisturiser in the daytime. Retinoids are not suitable during pregnancy and breastfeeding.
Topical antibiotics
Topical antibiotic treatments include clindamycin and erythromycin which are both safe to use in pregnancy. These work by reducing Propionibacterium/cutibacterium acnes as well as having a direct anti-inflammatory effect.
Antibiotics used alone whether topical or oral can create resistant strains of Propionibacterium/cutibacterium. For this reason, it is important to use antibiotics with either topical retinoids or benzyl peroxide to prevent antibiotic resistance.
Benzoyl peroxide
Benzoyl peroxide has been used for decades and is especially beneficial to an oily skin type as it causes further dryness and irritation with normal to dry skin. It also makes skin sun sensitive and bleaches clothing and towels. Benzoyl peroxide (5%) is recommended as first line therapy in mild adolescent acne and is safe to use in pregnancy.
Azelaic acid
20% Azeleic ( Skinoren) twice daily is effective in mild to moderate acne and especially suited to a dry skin as it is not irritating. Azeleic acid is also effective in reducing post inflammatory hyperpigmentation caused by acne lesions. It is safe to use during pregnancy and breastfeeding.
Topical combination treatments
Adapalene0.1% combined with 2.5% benzoyl peroxide (Epiduo) is an effective treatment for mild to moderate acne. It needs gradual introduction to minimise skin irritation. I recommend initiation of treatment twice a week for the first week, 3 times per week for second week and then every day once tolerated. It should be used at night with a good moisturiser to relieve dryness and sunscreen in the day.
This combination is also good for oily skin and excellent at reducing post inflammatory hyper-pigmentation.
Benzoyl peroxide 5% and clindamycin1% (Clindoxyl) is a topical treatment combining an antibiotic with benzoyl peroxide. This gel can therefore be used alone without resistance developing. It is suitable to treat both inflammatory lesion (papules and pustules) and non-inflammatory lesions (blackheads and whiteheads)
Systemic treatments
Systemic or oral medication is best for moderate to severe acne and widespread acne where it is difficult to treat all affected skin with topical medication.
Antibiotics
Adult facial acne responds very well to oral antibiotic treatments, but the problem is recurrence once the course is completed. Antibiotics should always be used in combination with a topical retinoid or benzoyl peroxide as the combined treatment prevents resistance, and has a synergistic effect which speeds up the response to treatment.
First line antibiotics for adolescent or adult acne are the tetracyclines. Commonly used in this class are lymecycline (Tetralysal ) and doxycycline. The once daily acne dosage greatly improves compliance.
Other antibiotics that can be used are erythromycin and sulfamethoxazole/trimethoprim combination (Purbac)
Hormones
Hormonal treatments are highly effective in treating adult female acne (they cannot be used in men).
As mentioned earlier they work even when there is no measured androgen excess and
have the added benefit of being suitable for long periods of use. For this reason, they are also a very good maintenance treatment.
When would I choose to prescribe a hormonal treatment?
First of all, the patient must not be pregnant, attempting to fall pregnant or breastfeeding and must be willing to take hormonal treatments. They work best when there is skin oiliness and premenstrual flare ups of acne and should ideally be combined with a topical retinoid, benzoyl peroxide, azelaic acid or antibiotic.
Cyproterone acetate
Cyproterone acetate is an anti-androgenic progesterone found either combined with oestrogen in the oral contraceptive pill (Diane -35, Minerva, Ginette) or alone at varying doses (Androcur).
It works by blocking the androgen receptor on the sebaceous glands preventing excessive sebum production. Side effects include mood swings, breast tenderness, fluid retention, nausea and vomiting.
Spironolactone
This potassium sparing diuretic also works by blocking the androgen receptors on sebaceous glands. It may cause increased potassium levels in those susceptible eg renal failure. It is however safe to use in young healthy women. It may be combined with the oral contraceptive pill, with the intrauterine contraceptive device or topical retinoids for added benefit.
Other combined oral contraceptive pills with antiandrogenic progesterone(drospirenone) eg Yaz, Yasmin. It is important to exclude risk of thromboembolism ie heart attacks and strokes when prescribing the oral contraceptive pill
Isotretinoin
Isotretinoin (roaccutane, oratane, acnetane, acnetret) is usually reserved for severe or resistant acne where other treatments have failed. It is also used in acne with significant scarring which deserves a more aggressive treatment approach. Isotretinoin works by reducing the size and activity of the sebaceous glands, improving keratinocyte shedding and reducing inflammation. Even though the results are undeniable, isotretinoin has many side effects which make many patients reluctant to take it unless absolutely necessary. The biggest problem with prescribing it in females is the risk of teratogenicity, which makes contraception essential in females at least while on the medication and 2-3 months after stopping treatment. Isotretinoin does not affect fertility. Other side effects include dryness of the lips, eyes, nose and other mucous membranes, dermatitis, joint and muscle pains. Isotretinoin can cause raised liver enzymes and raised cholesterol and triglycerides so baseline blood tests are needed before treatment and during the treatment period. Isotretinoin may also be associated with depressed moods. Despite all this it is still used frequently in adult acne especially after repeated courses of antibiotics and topical treatments prove to be unsuccessful. As with all other treatments of adult acne there is frequent relapse once treatment is discontinued. There are therefore many off label low doses used which are effective in treating acne while the patient is on the medication.
Cosmeceutical skincare
Acne treatments frequently cause dryness and skin irritation and may damage the epidermal skin barrier. This leads to increased transepidermal water loss (TEWL) and worsening of inflammation through triggering of the skin’s innate immunity. It is important to moisturise the skin and maintain the integrity of the epidermal barrier so that the treatment can be continued and the skin is comfortable without burning and peeling.
In addition to this cosmeceutical skincare has many ingredients that can help in the treatment of the acne. Ingredients like salicylic acid, lactic acid and glycolic acid help shed dead surface skin cells unblocking the opening of the hair follicle unit. This reduces the earliest lesion of acne, the microcomedone. Acne facewashes and toners can help reduce oiliness of the skin. Ingredients in skincare will also assist with reducing and treating post inflammatory hyperpigmentation and scarring which often remains long after the acne has been treated. Sunscreens protect against post inflammatory hyperpigmentation and counteract the sun sensitivity caused by many acne treatments.
It is important to note that skincare is ideally used together with prescription treatment in the case of active acne or plays a role in maintenance once the course of treatment is complete. A supportive skincare regimen is especially important in adult acne as the skin is not generally oily and thus more in need of hydration. Visit a dermatologist early for skin assessment and advice as delay in starting treatment can cause scarring to develop.
Procedures
Steroid injection of acne nodules is used for resistant painful inflammatory nodules or scarring nodules that fail to subside despite treatment. Injections can be carried out even during the course of treatment.
Comedone (blackhead and whiteheads) extraction may be necessary to speed up response to treatment. Open comedones(blackheads) are easier to remove, while closed comedones (whiteheads) may sometimes need very careful light cautery to open up the lesions. This will reduce the amount of inflammatory acne lesions forming and prevent trauma to the skin caused by picking if the patient is impatient and wants quicker results.
Chemical peels
Superficial chemical peels aid in superficial exfoliation and removal of dead surface skin cells which contribute to forming acne lesions. They are useful for acne with multiple comedones ( blackheads and whiteheads), to reduce inflammation in mild inflammatory acne and to improve post inflammatory hyperpigmentation and scarring. Glycolic, lactic, salicylic and pyruvic acid peels have been used.
Photodynamic therapy (PDT)
PDT has been used as an alternative treatment for acne. Amino levulanic acid (ALA) in a 10- 20% concentration is applied to the skin and red or blue light is shone on the skin to activate it. This treatment works as it’s anti-inflammatory. ALA penetrates into the follicular unit and on activation destroys Propionibacterium / cutibacterium acnes.
Dermal needling
This treatment is effective at remodelling the dermis and treating acne scarring and post inflammatory pigmentation effectively. It is best to start after active treatment is complete with a course of 6-8 sessions.
Conclusion
Adult acne is a challenge because its chronicity and significant impact on the quality of life of those that suffer from it. It perhaps becoming more and more prevalent. We don’t fully understand what causes it, though it seems the same pathogenetic mechanisms causing adolescent acne are at the root of it, with a whole range of contributing factors. It is critical to consult with your dermatologist sooner than later to discuss what treatment course is best suited to you. The management of adult acne is complex and there is no one size fits all perfect treatment, but acne can be controlled and managed with the correct guidance and tools.
You can have a look at our FREE online skin assessment that will help you get started , if you however would like to rather book a consultation to see Dr Kesiree Naidoo or the Skinsmart medical therapist, please do not hesitate to contact us on 021 531 1107 or email us on [email protected] or alternatively at [email protected]